![]()
UK Flexible Sigmoidoscopy Screening Trial
The UK Flexible Sigmoidoscopy Screening Trial (UKFSST) started in 1994 and is still on-going. The trial has received funding from a number of government and charitable sources including:
- the UK Medical Research Council
- the National Institute for Health Research (NIHR) Efficacy and Mechanism Evaluation programme
- the NIHR Health Technology Assessment programme
- Cancer Research UK
- KeyMed Ltd (now Olympus Ltd)
The UKFSST is a major research study and recruited over 170,000 people from across the UK. The main aim was to examine the effect of a once-only flexible sigmoidoscopy screening exam (a thin tube with a small camera on the end inserted through the rectum to examine the inside of the bowel) on the future risk of developing bowel cancer (also known as colorectal cancer) and the risk of dying from this cancer.
The first results assessing the effectiveness of the screening tested in this trial were published in 2010. The results confirmed that the test was very effective at preventing bowel cancer and very long-lasting. This study led directly to the introduction of flexible sigmoidoscopy (bowel scope/Flexi-scope) screening in the NHS English Bowel Cancer Screening Programme, which was announced by then Prime Minister David Cameron on 4th October 2010.
Harpal Kumar, Chief Executive of Cancer Research UK said of the UKFSST:
“Cancer Research UK does not often use the word ‘breakthrough’ but this is one of those rare occasions when I am going to. It is extremely rare to see the results of a clinical trial which are quite as compelling as this. Flexi-scope needs to be brought in as soon as possible. Every week of delay will risk scores of lives.”
Further results were published in 2017 that showed the protection from bowel cancer given by the screening test lasted at least 17 years.
In January 2021 the bowel scope procedure was withdrawn from the NHS Bowel Cancer Screening Programme in England. Despite its proven long-lasting protective effect against lower bowel cancer, a shortage of trained staff – endoscopists – to carry out the test meant that the screening procedure was never fully rolled out across the whole of England. This was further compounded by the COVID-19 epidemic and its disruption of endoscopy services, leading to flexible sigmoidoscopy as a screening method being officially stopped in England.
The trial is registered with the ISRCTN registry. Its unique number is 28352761.
Our Data Protection and Privacy Notice
This privacy notice explains your rights to your personal information, what you can expect us (the Cancer Screening and Prevention Research Group) to do with your personal data and our lawful basis for doing so. This notice also explains who you should contact if you have any queries or complaints about how we are processing your personal data.
Under the 2018 UK General Data Protection Regulation (GDPR) and accompanying Data Protection Act (2018) ‘personal data’ is any data that can be linked to an identifiable individual (for a full definition see: Information Commissioner’s Office [ICO] website: What is Personal Data?). Some types of personal data, such as health data, are additionally classified as ‘special category personal data’. The law considers special category personal data to be more sensitive and gives it more legal protection (for more information see: ICO website: Special Category Data). As the Cancer Screening and Prevention Research Group processes (processing is the term used to refer to collecting, analysing and storing data) health data, much of the personal data we hold is considered to be special category personal data.
Who is responsible for the lawful processing of your personal data?
The GDPR and Data Protection Act define roles and responsibilities for those involved in processing personal data.
The Cancer Screening and Prevention Research Group (hereafter; CSPRG) are a research group at Imperial College London. The CSPRG can be contacted via the ‘Contact Us’ page on this website. The data controller determines the purpose for which and the manner in which personal data is to be processed (see ICO website: Controllers and Processors). For the personal data held by the CSPRG, the data controller is Imperial College London. The data controller’s representative for our data is the Director of Information Governance for Academic Health Sciences. All queries relating to the handling of personal data should be directed to the Imperial College London Data Protection Officer via email at dpo@imperial.ac.uk. Contact details can also be found at the end of this privacy notice.
Why are we processing personal data?
The research focus of the CSPRG is gastrointestinal cancers which includes bowel cancer, also known as colorectal cancer. In the UK, every year around 42,900 people are diagnosed with bowel cancer alone and over 16,000 people die from this disease. Through our research we hope to reduce the number of people being diagnosed with gastrointestinal cancer and dying from this disease. Much of our work focuses on how to help make bowel cancer screening and surveillance programmes more effective and acceptable for patients, and more efficient for the NHS, and other health services internationally. To understand the effectiveness of bowel cancer screening and surveillance programmes, we conduct large scale studies on procedures conducted and the benefits to patients. Identifiable patient data are usually necessary to track long-term health outcomes from participants enrolled in our studies. The CSPRG therefore needs to collect and hold personal data – often special category personal data. Our more specific purposes for processing data for each of our studies are detailed on the ‘Studies’ pages of our website.
What personal data do we have?
The personal data we hold is special category personal data relating to individual health. For example, for several of our studies we analyse procedure and treatment information, information about cancers occurring, whether they progress and the patients’ long-term health outcomes. In addition, we also often require some basic information about patients such as age and gender to inform our analysis. The full details of the personal data processed for each of our studies can be found on the ‘Studies’ pages of our website.
To fulfil our research aims, we obtain personal data from a variety of sources. Much of our data is either obtained directly from NHS Trusts, or via national health data providers such as NHS England, the Office for National Statistics, the Bowel Cancer Screening Programme, national cancer registries such as Welsh Cancer Intelligence and Surveillance Unit, Public Health Scotland and NHS National Services Scotland. More detailed explanations of our sources of data can be found on the ‘Patient Data’ page and ‘Studies’ pages of our website.
Where data has been obtained from third-party data providers under section 251 of the National Health act 2006 approval, national data opt-outs have been applied by the provider since 2016.
How do we process personal data?
All personal data we hold are processed in secure systems. For each active study we have completed a Data Protection Impact Assessment that has been approved by the Head of the CSPRG (as the Information Asset Owner) and the Imperial College London Data Protection Officer. No processing performed by the CSPRG involves automated decision-making or profiling. Unless stated otherwise on the ‘Studies’ pages of our website, all personal data are processed by the CSPRG and certain third parties (see ‘Third-party processing’ below).
The Imperial College Data retention schedule mandates that data is retained for ten years after the end of a study (see Imperial’s Retention Schedule here). The expected end of these ten-year retention periods for each of our studies are listed under the ‘Studies’ pages of our website under the ‘How long will we retain the data?’ sections.
Third-party processing
For the purposes referred to in this privacy notice and relying on the bases for processing as set out above, we will share your personal data with certain third parties:
- Other Imperial College London employees, agents, contractors and service providers (for example, suppliers of printing and mailing services, email communication services or web services, or suppliers who help us carry out any of the activities described above). Our third-party service providers are required to enter into data processing agreements with us. We only permit them to process your personal data for specified purposes and in accordance with our policies.
What is our lawful basis for processing personal data?
Processing personal data requires justification under two legal frameworks: the UK GDPR/Data Protection Act 2018 and under the common law duty of confidentiality.
Article 6 of the UK GDPR lays out six valid bases under which personal data can be processed lawfully. We process personal data under lawful basis 6(1)(e) ‘Public task’ as: processing is necessary for the performance of a task carried out in the public interest. We are also required to have a separate lawful basis for processing the more sensitive special category personal data. Our legal basis for processing special category personal data is Article 9(2)(j) ‘processing is necessary for archiving purposes in the public interest, scientific or historical research purposes or statistical purposes […]’
In addition, health data (such as that the CSPRG hold) require a separate lawful basis under the common law duty of confidentiality. In some of our studies, patients consented to be part of the study and for the CSPRG to process their data. In other studies, consent could not be sought due to practical considerations or the nature of the study. In these studies, we have obtained lawful permission to obtain and process personal data under section 251 of the National Health Act 2006. The common law legal bases for data processing in each study are explained in the ‘Studies’ pages of our website under the ‘What approvals has the study received?’ sections.
What are your rights concerning your personal data?
The GDPR grants individuals several rights concerning their personal data:
- The right to object (to processing of the data)
- The right to correct (inaccurate or incomplete data)
- The right to erasure (also known as “the right to be forgotten”)
- The right to restrict processing (e.g. while the accuracy of the data is contested)
- The right to portability (to have a copy of any data you have provided to us)
- The right to access (to have a copy of data we hold about you)
- The right to withdraw consent (if you have previously consented to take part)
If you think that we might be processing your data and you wish to exercise any of the rights listed above, please get in touch using the details on the Contact Us page or by contacting the Imperial College London Data Protection Officer via email at dpo@imperial.ac.uk. Though it may not always be possible for us to fulfil your request, we will respond to your query within one month. For more information on your GDPR rights, please see guidance provided by the Information Commissioner’s Office.
Where can you direct queries or complaints?
Please be aware that individuals also have a right to complain to a supervisory authority – in this case the Information Commissioner’s Office (ICO) – if they feel their data is being used unlawfully. The ICO does recommend that you seek to resolve matters with the data controller – for our data that is Imperial College London – before contacting the Commissioner’s Office. If you wish to raise a complaint on how we have handled your personal data or if you want to find out more about how we use your data, please contact Imperial College London’s Data Protection Officer via email at dpo@imperial.ac.uk, via telephone on 020 7594 3502 or via post at Data Protection Officer, Faculty Building Level 4, Imperial College London, London SW7 2AZ.
If you are not satisfied with our response or believe we are processing your personal data in a way that is not lawful you can raise your complaint with the Information Commissioner’s Office. The ICO’s postal address is: Information Commissioner’s Office, Wycliffe House, Water Lane, Wilmslow, Cheshire SK9 5AF; Helpline number: 0303 123 1113. Other ways for members of the public to seek ICO advice can be found at https://ico.org.uk/global/contact-us/contact-us-public/public-advice/.
Privacy and data protection information relating specifically to the UKFSST study
The Cancer Screening and Prevention Research Group (CSPRG) at Imperial College London processes special category personal data for the UKFSST study. We use this special category personal data to examine the long-term effectiveness of a once-only flexible sigmoidoscopy. Effectiveness, in this case, refers to reduced incidence of bowel cancer, and a reduced chance of bowel cancer induced mortality. To determine this effectiveness, we need to process special category personal data relating to cancer incidence and mortality for participants enrolled in the trial. The special category personal data used in this study are crucial to the success of this project, and the public good generally.
Imperial College London, as data controllers for the CSPRG, are in receipt of special category personal data for the UKFSST. The special category personal data for the UKFSST are received by the CSPRG from several sources, given below.
1. NHS Hospitals
The flexible sigmoidoscopy procedures were carried out in NHS Hospitals in England, Scotland and Wales. These hospitals transferred the UKFSST trial data (i.e. the details of the procedure and relevant clinical data) to the CSPRG.
- Bolton Hospital, Bolton, and the Christie Hospital, Manchester
- John Radcliffe Hospital, Oxford
- Leeds General Infirmary, Leeds
- Leicester General Hospital, Leicester
- Norfolk and Norwich Hospital, Norwich
- Queen Alexandra Hospital, Portsmouth
- Queen Elizabeth Hospital, Birmingham
- Queen Elizabeth Hospital, Gateshead and Newcastle General Hospital, Newcastle upon Tyne
- Queen Elizabeth II Hospital, Welwyn Garden City
- Royal Liverpool Hospital, Liverpool
- St Marks Hospital, Harrow
- Royal Gwent Hospital, Newport and Llandough Hospital, Cardiff
- Singleton Hospital, Swansea
- Glasgow Royal Infirmary, Glasgow
2. NHS England
NHS England (formerly NHS Digital) collect and process data from across the health and social care system in England. For the UKFSST, NHS England provide the CSPRG with: cancer incidence and mortality for patients in England and Wales; cause of death data for patients in England and Wales (see Office for National Statistics below); and bowel cancer screening data for patients in England (see Bowel Cancer Screening Programme below). Some of these data are provided to NHS England from other sources, described below.
3. The Bowel Cancer Screening Programme
The Bowel Cancer Screening Programme manages screening tests for bowel cancer in England. The Bowel Cancer Screening Programme provide the CSPRG (via NHS England) with bowel cancer screening data for participants enrolled in the UKFSST study in England.
4. Office for National Statistics
The Office for National Statistics provide cause of death data for patients enrolled in this study from England and Wales. This information is provided to the CSPRG via NHS England.
5. The National Cancer Registration and Analysis Service
The National Cancer Registration and Analysis Service processes data about the progression and treatment of cancers in patients in England. Cancer incidence, mortality and staging data on UKFSST participants are provided to the CSPRG by the National Cancer Registration and Analysis Service.
6. Welsh Cancer Intelligence and Surveillance Unit
In Wales, cancer staging data is collected by the Welsh Cancer Intelligence and Surveillance Unit. For patients in Wales enrolled in the UKFSST, the Welsh Cancer Intelligence and Surveillance Unit provide cancer staging data to the CSPRG.
7. NHS National Services Scotland
The Information Services Division of NHS National Services Scotland manage the processing of health and care data in Scotland. For UKFSST participants in Scotland, NHS National Services Scotland provided the CSPRG with cancer incidence and mortality data, cancer staging data and cause of death data.
8. NHS Central Register
For UKFSST participants moving from England to Scotland during the trial, cancer incidence and mortality data, cancer staging data and cause of death data are provided to the CSPRG by the NHS Central Register.
No individual-level personal data from the UKFSST was transferred out of the CSPRG or Imperial College London.
What were the aims of the UKFSST?
The trial aimed to determine whether having a once-only flexible sigmoidoscopy screening test at around age 60 years was effective at preventing bowel cancer and could reduce the number of deaths from this disease. The trial also aimed to determine how long the benefit of the test lasted and the best age for it to be done.
What type of study was the UKFSST?
The UKFSST was a randomised controlled trial. People who participated in the trial were assigned randomly to receive either flexible sigmoidoscopy screening or the usual care that was offered at the time of the trial, which was no screening. Well-designed randomised controlled studies, such as the UKFSST, are considered to provide the best evidence for whether a new treatment works effectively.
What is the flexible sigmoidoscopy (bowel scope, Flexi-scope) test?
During flexible sigmoidoscopy (also called ‘bowel scope’ or Flexi-scope), a narrow, flexible tube with a camera on the end is inserted into the rectum and up into the lower part of the large bowel by a specialist nurse or doctor. Flexible sigmoidoscopy is used to examine the inner surface of the lower bowel for growths, called polyps or adenomas. Polyps are common and are not cancerous, but some can develop into cancer so they are generally removed as part of the procedure, or during a follow-up test.
When and where did the study take place?
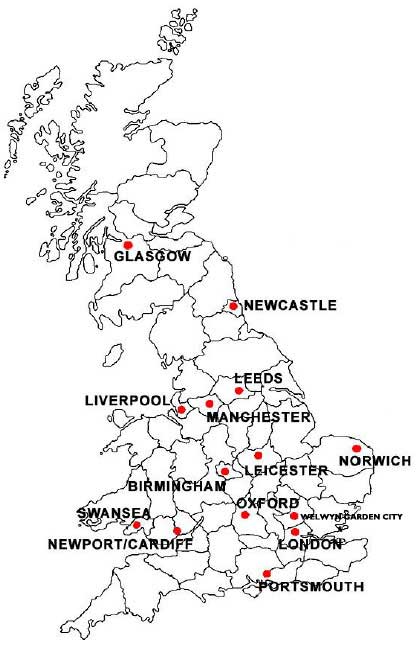
The UKFSST study recruited people from 506 participating GP practices based in 14 UK centres: 11 in England, two in Wales, and one in Scotland. The centres were located in Glasgow, Swansea, Newport/Cardiff, Newcastle, Leeds, Liverpool, Manchester, Birmingham, Leicester, Norwich, Oxford, Welwyn Garden City, London and Portsmouth (see map below).
Recruitment and screening started in November 1994 and were completed in March 1999.
Who is included in the study?
The 375,744 men and women who were assessed for eligibility for the UKFSST trial included those who:
- were registered at a participating GP practice between November 1994 and March 1999; and
- were aged 55–64 years between November 1994 and March 1999.
Of these, 170,432 people indicated in the study questionnaire or letter sent between September 1994 and March 1999 that they would take up the offer of screening if invited; were assessed as being eligible for the study; and were randomised. 40,621 of these 170,432 people were screened by flexible sigmoidoscopy.
The remaining 205,312 men and women included those who were judged as ineligible by their GP and not contacted and those who were sent a study questionnaire or letter between September 1994 and March 1999 asking whether they would take up the offer of screening if invited and:
- indicated that they would take up the offer of screening if invited and were eligible for the study but were not randomised as 40,000 people had already been screened (funding was given to screen 40,000 people); or
- indicated that they would take up the offer of screening if invited, but were subsequently assessed as not eligible for the study; or
- did not respond to the study questionnaire or letter; or
- responded to the study questionnaire or letter that they would not take up the offer of screening if invited.
What type of information does the CSPRG hold for the purposes of the UKFSST?
The CSPRG holds the following personal information for the purposes of the UKFSST, which covers:
- patient data– name, address, date of birth, NHS number, GP for all individuals in the age range 55-64 years between November 1994 and March 1999 belonging to participating general practices;
- questionnaire data – including responses to various questionnaires sent at different stages of the study, including information on family history of bowel cancer, symptoms, previous examinations and diet and smoking habits;
- clinical information – including medical data collected prior to screening, details of symptoms, results of any medical tests or procedures and blood samples;
- cancer diagnoses (for randomised patients) including histological diagnosis and stage of the disease;
- records of the deaths of individuals in the age range 55-64 years between November 1994 and March 1999 belonging to participating general practices.
We require the information that we hold in order to answer our research questions and to guarantee the quality and integrity of our results. It will not be possible to identify individuals from the published results of this study.
We have not finished collecting the cancer and death data we need and will continue to do so until March 2027. Our Patient Data section provides further details on what information we hold for the purposes of our research, and how we use and protect this information.
What approvals has this study received?
Everyone who received a flexible sigmoidoscopy as part of the UKFSST gave their consent for this procedure.
Consent was not sought from people who did not receive a flexible sigmoidoscopy as the group in question was extremely large (>335,000 people) and it was not possible to ask for consent from each individual. We received permission to conduct this research study from the independent ethical review committees and organisations responsible for the data of NHS patients, including:
- local research ethics committees in each of the 14 centres and the South-East multicentre research ethics committee;
- Section 251 approval from the Patient Information Advisory Group (PIAG – a predecessor of both the National Information Governance Board/NIGB and the Confidentiality Advisory Group) in England, and an equivalent panel in Scotland, the Privacy Advisory Committee (now the Public Benefit and Privacy Panel for Health and Social Care) of National Services Scotland (NSS);
- Research and Development approval from the NHS Trusts managing the centres involved in the trial;
- approval from the Caldicott Guardian of the North West London NHS Trust;
- approval from the UK Cancer Registries, NHS Digital, NHS Central Register (NHSCR), and the Office for National Statistics (ONS).
Why do we need to hold identifiable data for this study?
We need identifiable data to enable our data providers (such as NHS Digital, NHSCR, NSS, ONS, Cancer Registries and hospitals) to identify the study participants and provide us with follow-up data on cancers/deaths. We hold this data in the public interest (GDPR/DPA 2018: Article 6(1)e) for scientific research (GDPR/DPA 2018: Article 9(2)j)- please see the privacy notice for more information.
How long will we retain the data?
Our original funding allowed us to collect follow-up information on cancers and deaths for the UKFSST until March 2017. We have now been awarded additional funding to continue to follow-up the UKFSST cohort for a further 10 years until March 2027, until all the participants have reached the age of 80 years. Imperial College London, the organisation responsible for this study, requires that we hold data from all clinical studies for 10 years after the study end date. We therefore currently plan to hold the data for this study until March 2037.
What were the results of the study and what impact have they had?
When the first results of the UKFSST were analysed in 2010, they showed that people who were screened just once with flexible sigmoidoscopy (also known as bowel-scope) were:
- less likely to get bowel cancer – it prevented about one in three new cases of bowel cancer;
- less likely to die from the disease – it prevented four in every 10 deaths from bowel cancer.
The protective effects of once-only flexible sigmoidoscopy also appeared to be long lasting. The UKFSST results were published in The Lancet in 2010.
Because the UKFSST demonstrated that flexible sigmoidoscopy screening can prevent bowel cancer from developing, this suggested that offering a once-only flexible sigmoidoscopy (bowel-scope) screening test to people in the UK could reduce the numbers of people getting bowel cancer and dying from this disease. In 2010, the UK government announced a £60 million investment to introduce bowel-scope screening as part of the English NHS Bowel Cancer Screening Programme.
Roll-out of bowel-scope screening began in 2013. It has been estimated that bowel-scope screening could prevent up to 5,000 people from getting bowel cancer and up to 3,000 deaths from the disease in the UK each year. It is hoped that cancer of the rectum, the lowest part of the bowel examined, could one day become a rare disease.
The results of a further 7 years of follow-up were published in The Lancet in February 2017 and showed that a single flexible sigmoidoscopy continued to provide substantial protection from bowel cancer diagnosis and death, with protection lasting at least 17 years. News articles were also published by Cancer Research UK and by Imperial College London.
In addition to the original study objectives, we published a paper in 2020 that showed that having a better quality flexible sigmoidoscopy gives greater protection against getting bowel cancer or dying from it. Also, a 2018 publication looking at the use of stool tests in the BCSP among the UKSST participants found that those who were offered flexible sigmoidoscopy screening had lower rates of participation and outcomes, but that the use of stool tests could still be beneficial for everyone.
The UKFSST study team identified the following additional research questions which could be addressed by further analysis of the UKFSST dataset:
- Do patient experience and procedural factors affect the performance of flexible sigmoidoscopy screening?
- How safe and acceptable is a once-only flexible sigmoidoscopy?
- How does having a family history of bowel cancer affect the risk of developing this disease after screening?
- Can the severity of disease at diagnosis be used to determine the risk of dying from bowel cancer?
- Among patients identified as higher-risk at their flexible sigmoidoscopy screening, how effective is repeated colonoscopy (examination of the entire bowel) at routine intervals?
- How commonly does bowel cancer in the upper part of the large bowel develop after flexible sigmoidoscopy, and can this be predicted by the number and type of polyp detected at flexible sigmoidoscopy?
- Does smoking history affect the risk of developing polyps and bowel cancer?
- Can various medications affect the risk of developing polyps and bowel cancer?
- Among patients taking part in the UKFSST and also invited to complete a stool test as part of the National Bowel Cancer Screening Programme (BCSP), how do these two screening tests affect the risk of getting bowel cancer?
These analyses will be conducted by the CSPRG research team and published in peer reviewed journals. No additional data will be requested to meet these objectives.
Publications
Wooldrage K*, Robbins EC, Duffy SW, Cross AJ. Long-term effects of once-only flexible sigmoidoscopy screening on colorectal cancer incidence and mortality: 21-year follow-up of the UK Flexible Sigmoidoscopy Screening randomised controlled trial. Lancet Gastroenterol Hepatol 2024; 9: 811–24. doi: 10.1016/S2468-1253(24)00190-0.
Power S*, Wooldrage K, Saunders BP, et al. The impact of endoscopist performance and patient factors on distal adenoma detection and colorectal cancer incidence. BMC Gastroenterol 24, 44 (2024). doi:10.1186/s12876-024-03125-x.
Robbins EC, Wooldrage K, Saunders BP, Cross AJ. PP0980 (Poster) Long-term colorectal cancer incidence, unperturbed by surveillance, among people with no polyps and those with low-risk polyps: an analysis of data from the UK Flexible Sigmoidoscopy Screening Trial. UEG Week 2023; 11(S8):1103-1104. doi:10.1002/ueg2.12461.
Juul FE, Cross AJ, Schoen RE, et al; 15-Year Benefits of Sigmoidoscopy Screening on Colorectal Cancer Incidence and Mortality: A Pooled Analysis of Randomized Trials. Ann Intern Med. 2022;175:1525-1533. [Epub 11 October 2022]. doi:10.7326/M22-0835.
Robbins EC, Wooldrage K, Stenson I, Pack K, Duffy S, Weller D, Levin T, Conell C, Wright S, Nickerson C, Martin J, Cross AJ*. Heterogeneity in colorectal cancer incidence among people recommended 3-yearly surveillance post-polypectomy: a validation study. Endoscopy. 2021 Apr;53(4):402-410. doi: 10.1055/a-1217-0155.
Robbins EC*, Wooldrage K, Saunders BP, Duffy SW, Cross AJ. P22 (Poster) Impact of adenoma detection rates at flexible sigmoidoscopy on long-term colorectal cancer incidence and mortality. doi:10.1136/gutjnl-2020-bsgcampus.97 BSG Virtual campus conference Jan 2021.
Brenner H*, Cross AJ. Merits, Challenges, and Limitations of Randomized Trials on Colorectal Cancer Screening Effectiveness. Gastroenterology. 2021 Mar;160(4):1009-1011. doi: 10.1053/j.gastro.2020.12.029.
Cross AJ, Robbins EC, Saunders BP, Duffy SW, Wooldrage K. Higher adenoma detection rates at screening associated with lower long-term colorectal cancer incidence and mortality. Clin Gastroenterol and Hepatol. 2020. doi: 10.1016/j.cgh.2020.09.020.
Pinsky PF, Loberg M, Senore C, Wooldrage K, Atkin W, Bretthauer M, Cross AJ, Hoff G, Holme O, Kalager M, Segnan N, Schoen RE. Number of Adenomas Removed and Colorectal Cancers Prevented in Randomized Trials of Flexible Sigmoidoscopy Screening. Gastroenterology. 2018 Jun 20. pii: S0016-5085(18)34667-5. doi: 10.1053/j.gastro.2018.06.040.
Brown JP, Wooldrage K, Kralj-Hans I, Wright S, Cross AJ, Atkin WS. Effect of once-only flexible sigmoidoscopy screening on the outcomes of subsequent faecal occult blood test screening. J Med Screen. 2018 Oct 3:969141318785654. doi: 10.1177/0969141318785654.
Atkin W, Wooldrage K, Parkin DM, et al. Long term effects of once-only flexible sigmoidoscopy screening after 17 years of follow-up: the UK Flexible Sigmoidoscopy Screening randomised controlled trial. Lancet. 2017 Apr 1; 389 (10076): 1299-1311.
McGregor LM, Bonello B, Kerrison RS, et al. Uptake of Bowel Scope (Flexible Sigmoidoscopy) Screening in the English National Programme: the first 14 months. J Med Screen. 2016 Jun;23(2):77-82.
Robb KA, Lo SH, Power E, et al. Patient-reported outcomes following flexible sigmoidoscopy screening for colorectal cancer in a demonstration screening programme in the UK. J Med Screen 2013: 1–6.
Robb K, Power E, Kralj-Hans I, et al. Flexible sigmoidoscopy screening for colorectal cancer: Uptake in a population-based pilot programme. Journal of Medical Screening. 2010;17(2):75-8.
Atkin WS, Edwards R, Kralj-Hans I, et al. Once-only flexible sigmoidoscopy screening in prevention of colorectal cancer: a multicentre randomised controlled trial. Lancet. 2010; 375: 1624–33.
Austin KL, Power E, Solarin I, et al. Perceived barriers to flexible sigmoidoscopy screening for colorectal cancer among UK ethnic minority groups: a qualitative study. J Med Screen 2009; 16: 174–179.
Miles A, Atkin WS, Kralj-Hans I, et al. The psychological impact of being offered surveillance colonoscopy following attendance at colorectal screening using flexible sigmoidoscopy. J Med Screen 2009; 16(3): 124-130.
Robb KA, Power E, Atkin W, et al. Ethnic differences in participation in flexible sigmoidoscopy screening in the UK. J Med Screen 2008; 15: 130-136.
Brotherstone H, Vance M, Edwards R, et al. Uptake of population based flexible sigmoidoscopy screening: a nurse-led feasibility study. J Med Screen 2007;14:76-80.
Mitrou PN, Loktionov A, Atkin W, et al. MTHFR C677T and A1298C polymorphisms and risk of colorectal adenoma in the UK Flexible Sigmoidoscopy Trial. (United Kingdom). Cancer causes control. 2006 Aug;17(6):793-801.
Thomas-Gibson S, Rogers, PA, Cooper S, et al. Judgement of quality of bowel preparation at screening flexible sigmoidoscopy is associated with variability in adenoma detection rates. Endoscopy. 2006;38:456-60.
Gunter MJ, Watson MA, Loktionov AS, et al. No association between cytochrome P450 and Glutathione S-Transferase gene polymorphisms and risk of colorectal adenoma: results from the UK flexible sigmoidoscopy screening trial. Cancer Epidemiology Biomarkers Prev. 2005;14(4):1028-30.
Atkin WS, Rogers P, Cardwell C, et al. Wide variation in adenoma detection rates at screening flexible sigmoidoscopy. Gastroenterology 2004;126:1247-56.
Miles A, Wardle J, Atkin W. Receiving a screen-detected diagnosis of cancer: the experience of participants in the UK flexible sigmoidoscopy trial. Psycho Oncology. 2003;12:784-802.
Adams C, Atkin WS, Cardwell C, et al. Effect of hysterectomy status on polyp detection rates at screening flexible sigmoidoscopy. Gastrointest Endosc. 2003;57(7):848-53.
Whynes DK,Frew EJ, Atkin WS. The costs of flexible sigmoidoscopy screening for colorectal cancer. Int J Technol Assess Health Care. 2003;19(2):384-95.
Atkin WS, Cook C, Cuzick J, et al. Single flexible sigmoidoscopy screening to prevent colorectal cancer; baseline findings of a UK multicentre randomised trial. Lancet. 2002;359:1291-300.
Atkin WS, Edwards R, Wardle J, et al. Design of a multicentre randomised trial to evaluate flexible sigmoidoscopy in colorectal cancer screening. J Med Screen. 2001; 8:137-44.
McCaffery K, Borrill J, Williamson S, et al. Declining the offer of flexible sigmoidoscopy screening for bowel cancer: a qualitative investigation of the decision-making process. Soc Sci Med. 2001;53:679-91.
Wardle J, Sutton S, Williamson S, et al. Psychosocial influences on older adults interest in participating in bowel cancer screening. Prev Med. 2000;31:323-34.
Sutton S, Wardle J, Taylor T, et al. Predictors of attendance in the UK flexible sigmoidoscopy screening trial. J Med Screen. 2000;7:99-104.
Martin JP, Sexton BF, Saunders BP, et al. Inhaled patient-administered nitrous oxide/oxygen mixture does not impair driving ability when used as analgesia during screening flexible sigmoidoscopy. Gastrointest Endosc. 2000;51:701-3.
Taylor T, Williamson S, Wardle J, et al. Acceptability of flexible sigmoidoscopy screening in older adults in the UK. J Med Screen. 2000;7:38-45.
Atkin WS, Hart A, Edwards R, et al. Single blind, randomised trial of efficacy and acceptability of oral picolax versus self-administered phosphate enema in bowel preparation for flexible sigmoidoscopy screening. Br Med J. 2000;320:1504-9.
Bell GD, Atkin WS, Painter J, et al. Increasing the reach of flexible sigmoidoscopy. Endoscopy. 1999;31:835.
Frew E, Wolstenholme JL, Atkin WS, et al. Estimating time and travel costs incurred in clinic-based screening: flexible sigmoidoscopy screening for colorectal cancer. J Med Screen. 1999;6:119-23.
Wardle J, Taylor T, Sutton S, et al. Does publicity about cancer screening raise fear of cancer? Randomised trial of the psychological effect of information about cancer screening. Br Med J. 1999;319:1037-8.
Hart AR, Kudo S, Mackay EH, et al. Flat adenomas exist in asymptomatic people: important implications for colorectal cancer screening programmes. Gut. 1998;43:229-31.
Atkin WS, Hart A, Edwards R, et al. Uptake, yield of neoplasia and adverse effects of flexible sigmoidoscopy. Gut. 1998;42:560-5.
Atkin W. Flexible sigmoidoscopy as a mass screening tool. Euro J Gastroenterol Hepatol. 1998;10:219-23.
